With the UK’s ageing population and growing demand for home-based healthcare, domiciliary optometry is emerging as a vital and rewarding career path. As more patients face mobility challenges due to age, disability, or health conditions, the need for skilled optometrists delivering care outside the high street continues to rise. Whether you’re newly qualified or a seasoned professional seeking change, this guide offers a comprehensive look at the skills, rewards, and opportunities available in domiciliary eye care.
Domiciliary optometry involves delivering full-scope eye care services in patients' homes, residential facilities, or care homes. This mobile service enables patients who are housebound or unable to travel to receive essential sight tests and professional care.
This field is especially impactful for the elderly, individuals with low vision, and those in long-term care, ensuring continuity of eye care regardless of physical limitations.
Domiciliary eye care offers a compelling blend of flexibility, autonomy, and impact. Optometrists in this field often cite greater job satisfaction due to strong patient relationships and the ability to work Monday to Friday with more predictable hours.
Many domiciliary roles offer well-structured programmes with competitive salaries, access to professional support, and use of a company vehicle. Additionally, there are increasing opportunities for entrepreneurial optometrists to take part in service development, team leadership, or shared ownership models.
With the ongoing expansion of community-based healthcare and increased focus on reaching underserved populations, career opportunities in domiciliary optometry continue to grow across the UK.
Qualifying as a domiciliary optometrist involves a multi-step process:
Begin with a General Optical Council (GOC)-approved undergraduate degree in optometry from a UK university.
Following your degree, complete a structured pre-registration year under the supervision of a qualified optometrist. This includes practical assessments and the College of Optometrists’ final Scheme for Registration.
Once all pre-registration requirements are met, you must register with the GOC to practice legally as an optometrist in the UK.
Although not mandatory, training in safeguarding, dementia awareness, low vision, and manual handling is highly recommended to prepare for work with vulnerable populations.
Securing the right role is a pivotal step. Partnering with a Verovian Optical Recruitment Agency will significantly streamline this process, connecting optometrists with suitable and growth-orientated employers.
Most domiciliary employers offer comprehensive onboarding programmes that include practical training in the use of mobile equipment, patient communication strategies, lone worker safety, and daily logistics.
This pathway ensures that optometrists entering domiciliary care are clinically competent, practically prepared, and well-supported to deliver high-quality care in non-traditional settings.

In addition to core clinical competencies, domiciliary optometrists require a specialised skill set, including:
A domiciliary optometrist’s day revolves around visiting patients in their homes or care facilities, providing full eye exams and clinical assessments equivalent to those in a traditional clinic. They deliver expert care on the go using portable and specialised tools such as
Most employers provide this essential equipment, ensuring optometrists have access to the latest technology. Often accompanied by an optical assistant, they manage everything from patient care to dispensing glasses, making the process seamless and efficient.
After each visit, findings are carefully recorded and shared with the clinical team to guarantee ongoing patient support.
Gaining insight through shadowing an experienced domiciliary optometrist or exploring part-time roles is a great way to get started.
Further professional development can include:
While the role is fulfilling, it also comes with specific challenges:
Despite these, the rewards are significant. Offering personalised eye care to those unable to access traditional services provides emotional and professional fulfilment. The relationships built, flexibility achieved, and societal contribution made often outweigh the logistical difficulties.
Domiciliary optometry presents a distinctive and meaningful career within the broader eyecare profession. It offers a blend of clinical independence, personal fulfilment, and the chance to reach patients who need it most. Whether you’re exploring new challenges or seeking a more flexible, patient-focused role, domiciliary eye care may be the next step in your professional journey.
Ready to step into a rewarding career in domiciliary optometry? At Verovian Optical Recruitment Agency, we connect qualified optometrists with flexible, high-impact roles across the UK. Whether you're newly registered or looking for a fresh start, we’ll help you find the right fit. Start your journey with us today – Register now.
The NHS in England is undergoing a major transformation in 2025, reshaping how health services, particularly eye care, are delivered. With rising demand for hospital eye services and a pressing need to reduce waiting times, these reforms mark a pivotal step in ensuring the NHS is fit for the future.
This blog offers an up-to-date overview of the key pillars of the NHS 2025 eye care reforms, explores what they mean for optical practices and professionals today, and provides practical advice for adapting to this new landscape.
The NHS Eye Care Reforms 2025 are a set of nationally coordinated changes aimed at transforming how eye health services are delivered across England. Aligned with the NHS Long Term Plan, these reforms are designed to move services from overstretched hospital settings to more accessible community optical practices, making care more local, preventative, and efficient. By prioritising primary care and elective care access, the reforms aim to reduce wait times, improve patient outcomes, and support a transition from sickness to prevention. This updated model of care ensures NHS services are fit for the future, using community-based providers to deliver timely, high-quality care.
Established in April 2025, this pillar standardises urgent and emergency eye care across England. Led by NHS England and the College of Optometrists, it shifts care closer to home, easing hospital eye service demand and improving patient access and outcomes across the NHS.
Central to the 2025 health plan, this reform empowers optical practices to deliver urgent and elective eye care services previously provided in secondary care. Supported by NHS England, Integrated Care Boards, and Local Optical Committees, it strengthens primary care providers and promotes proactive, integrated care aligned with the NHS mandate.
Published in January 2019, the integration of primary and community care is an ongoing NHS development and a key pillar of the 2025 eye care reforms. Led by NHS England and Integrated Care Boards under the Department of Health and Social Care’s mandate, it aims to shift care from sickness to prevention, making health and social care more fit for the future.
As part of the 2025 reforms, expanding NHS optical voucher uptake improves access to essential eye care, especially among vulnerable populations. Streamlined eligibility and processes ensure equitable care delivery and support the government’s investment in NHS eye care to reduce health inequalities across England.
NHS England’s commitment to enhanced training equips optical professionals with the skills to manage urgent and minor eye conditions. This supports the expanded model of care by building a workforce capable of delivering high-quality eye care services closer to patients and reducing pressure on hospital eye services.
Critical to the reforms, upgrading optical practices’ systems to the NHS digital infrastructure enables electronic referrals and shared records. This digital integration facilitates coordinated care delivery, improves patient flow through eye care services, and supports the NHS’s broader move from analogue to digital health and social care.
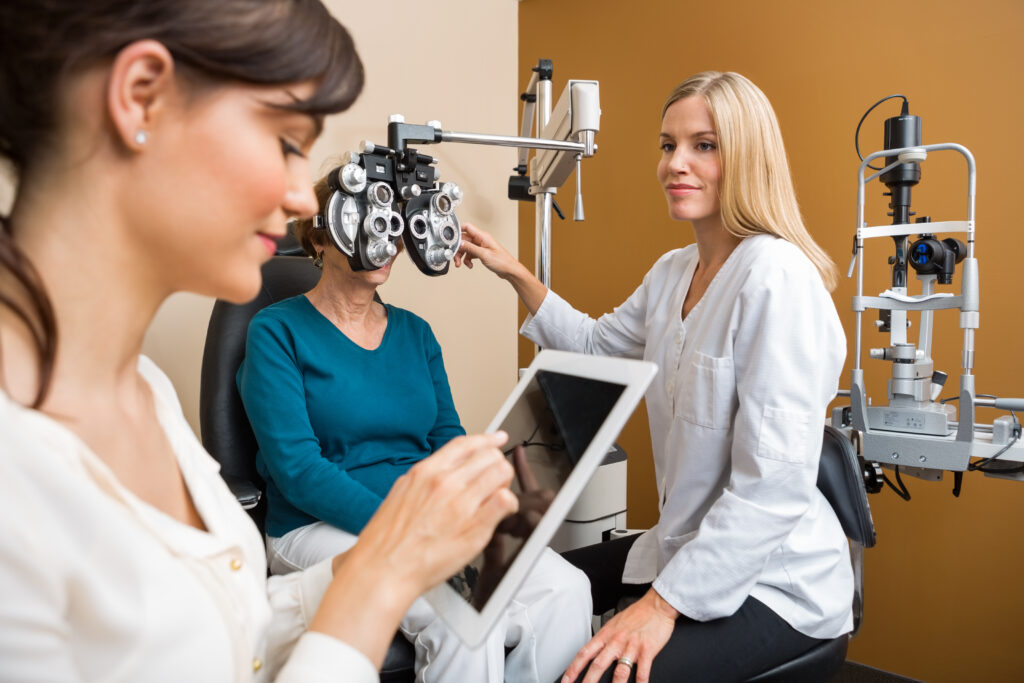

The 2025 NHS Eye Care Reforms represent a critical opportunity for optical practices and professionals to lead in delivering accessible, preventative eye care. By embracing integration, digital innovation, and expanded clinical roles, the optical sector can meet rising demand, improve patient outcomes, and strengthen its position within the NHS.
These reforms create a pathway for optical practices to become integral to community eye care, thereby reducing hospital pressures and enhancing patient access. Practices that invest in digital infrastructure, workforce development, and collaborative networks will be best placed to thrive in this evolving landscape. Just so you know, the time to act is now. Position your practice and your team to meet the future of NHS eye care.
Partner with us for expert optical recruitment solutions. We connect practices with top professionals, helping you grow, innovate, and deliver exceptional eye care across NHS England in 2025 and beyond.
For internationally trained optical professionals, the UK presents exciting career opportunities in a well-respected healthcare system. However, before you can practice as an optometrist, you must be registered with the General Optical Council (GOC). This registration ensures that all professionals meet consistent standards in patient care and clinical practice.
In this blog post, we’ll walk you through the GOC registration process, explain the eligibility requirements, and provide tips to help you transition smoothly into the UK optical workforce.
The General Optical Council (GOC) regulates optometrists and dispensing opticians in the UK. Its mission is to protect the public by maintaining education, performance, and professional conduct standards. As an overseas‑qualified optometrist, GOC registration is mandatory—without it, you cannot legally examine eyes, prescribe lenses, or work in any UK optical practice.
To qualify for GOC registration, you must demonstrate that your overseas optometry education and clinical experience align with UK requirements. Specifically, you will need to show:

First, complete the self‑assessment form. A response will arrive by email within three working days, detailing any required documentation and, if eligible, the application form.
Before submitting your application form to the GOC, verify your qualifications through the Qualification Check (QC) using the link in your application email. This service carries a fee—see the QC website for current pricing. Follow the the step‑by‑step guide to complete the QC.
Once all required documents are received and your application is approved, you will be required to pay the assessment fee, which must be paid within 14 days.
If invited to interview, the interview fee must be paid within 14 days.
You will be notified of the outcome in writing. Possible outcomes:
The Scheme for Registration is the UK’s pre‑registration pathway for internationally trained optometrists. It helps you build the practical skills and knowledge you need in a UK workplace before achieving full GOC registration.
This comprises three parts:
Stage 1 and Stage 2 Work‑Based Assessments – Ongoing evaluations of your clinical competencies on the job.
Objective Structured Clinical Examination (OSCE) – A final practical exam that tests your hands‑on skills and decision‑making.
It takes up to two years and three months to complete the entire Scheme, although most trainees finish within about 15 months.
1. Apply online via the GOC website, but ensure you fill out the application identification form before you complete the application form.
2. Upload Documents: The completed application form and supportive documents should be emailed to [email protected].
3. Pay the Required Fee: As part of the international optometry registration process, you’ll be required to pay the following fees within 14 days of receiving each invoice:
£205 – Interview fee
£130 – Document scrutiny
£455 – Application assessment
4. Receive your GOC Registration Number and join the UK register of optometrists.
Stay Informed: Regularly check the GOC website for updates to OBS modules or exam format.
Becoming a GOC‑registered optometrist is your gateway to practising in the UK’s dynamic optical sector. While the process demands careful preparation—qualification assessment, possible bridging, pre‑registration practice, and final examination—thousands of international optometrists have successfully made the transition.
At Verovian Optical Agency, we specialise in connecting passionate and qualified optometrists with exciting opportunities across the UK. Whether you're just starting out or looking to take the next step in your career, our expert recruitment team is here to match you with roles that suit your skills, interests, and aspirations. We understand the optical sector inside and out, offering tailored guidance and ongoing support to ensure you thrive in your new position. From locum placements to permanent roles, we’re committed to helping you build a successful and fulfilling career in optometry. Ready to take the next step? Register with Verovian Optical Agency today and let us help you find your perfect role.
Working with children in an optical setting can be one of the most rewarding—and at times, most challenging—parts of an optometrist’s day. A young patient may walk in feeling shy, confused, or even fearful of what’s to come. For many, it’s their very first eye exam. That’s why mastering effective communication skills isn’t just helpful—it’s essential.
In this guide, we’ll explore practical strategies to help optometrists enhance their communication with paediatric patients, building trust, easing anxiety, and creating a positive experience that sets the foundation for lifelong eye health.
Children aren’t simply smaller versions of adults—they experience the world, and healthcare, in entirely different ways. Their communication skills are still developing, which often makes it difficult for them to articulate visual discomfort or specific symptoms. As a result, optometrists must adopt a flexible, child-centred approach that relies not only on verbal communication but also on keen observation and rapport-building. Being alert to unspoken signals —such as fidgeting, changes in facial expression, or avoiding eye contact—can often provide more insight than words alone.
To create a more accurate clinical picture, it's essential for a parent or carer to be present during the examination. They can provide key information and provide reassurance that helps the child feel more at ease. Ultimately, patience, empathy, and a genuine interest in the child’s well-being are key to successful paediatric eye examination and care. By understanding a child’s developmental stage and emotional needs, optometrists can build trust and foster cooperation, ensuring the experience is as positive and productive as possible.
The setting itself can make or break a child’s experience. A stark, clinical room may feel intimidating, whereas a bright, engaging space immediately puts young patients at ease and lays the groundwork for trust.
A welcoming atmosphere speaks louder than any reassurance you can offer verbally.
Children require a tailored approach, depending on their age and developmental stage:
This age-appropriate approach builds confidence and cooperation across all age groups.
One of the most effective ways to ease anxiety when examining children is to make the equipment and procedures feel familiar. Children feel more confident and cooperative when they understand what’s happening, especially if it’s explained in a fun, relatable way. Try using simple analogies like, “This is a camera that takes pictures of your eyes,” or “This machine plays a secret light game to check how well your eyes work.” Phrasing it like a game or adventure often sparks curiosity instead of fear.
Whenever possible, get the child involved. Let them press a button, hold a torch, or explore a mirror. Demonstrating a procedure on a toy or stuffed animal before doing it on the child can also be hugely reassuring. These small gestures turn a clinical experience into something playful and empowering, making the appointment feel less intimidating for the child and their carer.
Fear of the unknown is common among children. Soften their concerns by:
The goal is to make the visit feel less like an exam and more like an adventure.

While your primary focus is the child, their parent or guardian is an essential partner in the process. Keeping them informed and involved not only reassures them but also helps reinforce your clinical advice beyond the practice. Use clear, simple language to explain your findings and the next steps, making sure they feel confident about what’s happening. Encourage parents to support good visual habits at home—like limiting screen time or promoting regular eye breaks—and invite them to help if their child is particularly anxious or reserved. When the child, parent, and optometrist work together as a team, it creates a more supportive and effective environment for paediatric eye care.
Communication is an evolving skill, and reflection is key to improving. After each paediatric consultation, take a few moments to reflect on what worked well and what didn’t. Did you effectively engage the child? Were you able to explain complex procedures in a way they could understand? Reflecting on your approach helps you build a stronger, more adaptable communication style.
Communication is a clinical skill, and like any other, it can be honed over time. For optometrists, particularly if you're working with children, investing in this skill can transform how your patients experience care. Strong communication builds trust, reduces anxiety, and leads to better cooperation during eye exams. With the right training and tools, you can refine your approach and make every paediatric consultation smoother and more effective. Here are some practical ways to invest in your communication skills:
Look for CPD opportunities that cover communication techniques specifically tailored to children. Association of optometrists, Optometry Today, and The College of Optometrists offer a range of learning modules and events that explore behavioural strategies and practical methods for working with younger patients—ideal for refining your approach in paediatric settings.
Your Local Optical Committee (LOC) is a valuable source of ongoing support and education. By attending LOC meetings or workshops, you can engage in peer discussions, share practical tips, and learn effective communication strategies from fellow optometrists who regularly work with children.
Understanding how children communicate at different developmental stages can guide your approach. Online platforms such as FutureLearn offer a flexible, evidence-based way to learn about this.
Being an optometrist isn’t just about diagnosing refractive errors or prescribing glasses—it’s about making children feel seen, heard, and safe. By enhancing your communication skills, you not only improve the quality of the eye exam but also help shape a child’s long-term attitude towards healthcare. A successful interaction today could be the reason that same child returns years later as a confident, responsible adult who prioritises their vision health.
Whether you're just starting out in the optical industry or ready to take your career to the next level, Verovian Optical Agency is here to support you. We specialise in connecting optical professionals with a wide range of exciting locum and permanent roles across the UK in opticianry, optometry, and ophthalmology. With tailored opportunities that align with your skills and passion, we make sure you find a role that suits your career aspirations. Register with us today, and let’s work together to find your next career move!
Mark your calendars! From March 17th to 23rd, 2025, the global eye care community will celebrate World Optometry Week, culminating in World Optometry Day on March 23rd. The World Council of Optometry (WCO) has unveiled the powerful theme, "Eyes to the Future: Optometry Improving Global Wellness." This theme underscores the transformative impact of optometry in building a healthier world. From preventing vision loss to pioneering cutting-edge technologies, optometry is redefining healthcare, ensuring clear vision and fulfilling lives for everyone. Join us as we explore the evolving landscape of optometry, the innovations driving change, and the strides being made toward global access to quality vision services.
Optometry's impact extends far beyond simple vision correction. It's a cornerstone of global healthcare, contributing significantly to overall wellness, disease prevention, and the detection of systemic health conditions. Think of it as a vital entry point within broader health systems. The World Council of Optometry (WCO) celebrates the tireless efforts of optometrists worldwide, who are actively breaking down barriers to care by expanding access, educating patients, and advocating for seamless integration of eye care into global health systems.
"As an optometrist and the President of WCO, I am proud to see how the care we offer our patients helps lead to increased awareness of health issues, more involvement in prevention of vision and overall health problems, along with early diagnosis, quality eyecare, and integration of vision and eye health as a part of universal health care," states WCO President Sandra Block.
With millions globally facing preventable vision impairment, optometry's role in ensuring equitable access to quality eye care, particularly in underserved regions, is more critical than ever.

Looking ahead, optometry's role in global healthcare is poised to become even more vital. The increasing global population, coupled with an ageing demographic and rapid urbanisation, presents considerable challenges for healthcare systems, especially in delivering sustainable eye care.
Optometry is uniquely positioned to lead the way in addressing these challenges. By expanding its role as a primary eye care provider within collaborative care models, optometrists are evolving their education and training to encompass not just vision correction but also the investigation, monitoring, and treatment of a wide range of eye diseases.
The WCO Competency Framework for Optometry, launched in March 2024, underscores the competencies needed for optometry to effectively participate in the international eye care agenda. This expanded scope is essential for meeting the growing demand for eye care, particularly in community or hospital settings with limited access. By integrating optometrists into multidisciplinary healthcare teams, countries can significantly improve the prevention and treatment of eye diseases and better serve their populations.
The WCO urges optometrists, healthcare leaders, and policymakers worldwide to prioritise eye care within the global health agenda.
"Through collaboration, innovation, and continued education, the global optometry community is preparing for the future, ensuring that the eyes of tomorrow are in capable hands," the organisation emphasises.
Optometry is about more than just sight; it's about transforming lives. On World Optometry Day 2025, we honour the professionals dedicated to enhancing eye health and champion universal access to quality vision care.
For those passionate about the future of optometry and eager to explore new opportunities, Verovian Optical Recruitment Agency is here to connect you with the right role. Register with us today to stay informed about the latest advancements and opportunities in the field.

In today’s rapidly evolving healthcare landscape, diversity and inclusion are more than just buzzwords—they’re strategic imperatives that can drive success in any optical practice. With the UK’s demographic makeup continually shifting, it’s essential for optical practices to not only recognise but also embrace the rich variety of backgrounds, perspectives, and experiences among their patients and staff.
In this post, we explore why diversity and inclusion (D&I) matter in optics and provide practical strategies for UK optical practice owners to integrate these initiatives into their day-to-day operations.
Diversity and Inclusion (D&I) in optics refers to the intentional efforts made by optical practices and businesses to create a workforce and patient experience that reflects and respects differences in race, gender, age, disability, socioeconomic background, and more. It ensures that both employees and patients are valued, heard, and provided with equitable opportunities and care.

Expanding your candidate pool is essential for building a diverse and inclusive optical practice. To attract a wider range of talent, advertise vacancies on platforms that reach diverse candidates and ensure inclusive hiring practices. Additionally, adopting blind recruitment—removing personal identifiers such as names and backgrounds from applications—helps eliminate unconscious bias, ensuring that hiring decisions are based solely on skills, experience, and qualifications. Partnering with a trusted recruitment agency like Verovian Optical Recruitment Agency can further streamline this process, connecting you with a diverse pool of highly qualified optical professionals while ensuring fair and inclusive hiring practices.
Create an environment where all employees feel welcomed and valued. This involves more than just hiring a diverse team; it means fostering a culture that actively supports and includes diverse perspectives. Encourage open dialogue, respect different viewpoints, and ensure that all staff members have a voice in decision-making processes.
Actively celebrating diversity within your optical practice is a powerful way to promote inclusivity and build a positive workplace culture. For example, recognising and celebrating cultural events such as Black History Month, Diwali, or Eid can help make all staff and patients feel seen and respected. You could also highlight the unique contributions of employees from different backgrounds, perhaps through spotlight features or internal awards. By promoting such inclusivity, your practice not only boosts employee morale but also shows patients that your practice is truly committed to equality and representation.
Investing in employee training and development is key to fostering a diverse and inclusive optical practice. Regular cultural competency workshops can help staff understand different cultural perspectives, address unconscious bias, and improve patient interactions. Additionally, implementing mentorship programmes provides valuable support for all employees, particularly those from underrepresented backgrounds, helping them develop their skills and progress in their careers. By prioritising continuous learning and professional growth, your practice can create a more inclusive workplace while enhancing the quality of patient care.
Establishing clear inclusion policies is essential for creating an equitable environment within your optical practice. These policies should promote fairness and inclusion at every level, ensuring that they are actively implemented and not just written guidelines. Additionally, it's important to conduct a regular review of your diversity and inclusion initiatives. Continuously assessing the effectiveness of these strategies, along with being open to feedback and adapting to changing needs, helps ensure your practice stays aligned with its D&I goals and creates a truly inclusive workplace.
Building local partnerships with community groups is a valuable way to understand the specific needs of diverse populations and tailor your optical services accordingly. By connecting with these groups, you can create more inclusive, accessible offerings that resonate with their unique needs. Additionally, gathering patient feedback on a regular basis is crucial for refining your services. Actively listening to your diverse patient base and using their insights helps ensure that your practice continually improves and remains responsive to the needs of all patients, fostering a more inclusive and patient-centered environment.
The evidence is clear: diversity and inclusion initiatives are not just ethical imperatives—they are also powerful drivers of business success. From enhancing patient care to fostering innovation and boosting staff morale, the benefits are manifold. For UK optical practice owners, the time is now to evaluate your current strategies and commit to a more inclusive approach.
By taking proactive steps to implement D&I initiatives, you can create a more welcoming environment for both your patients and your team, ultimately positioning your practice for long-term success.
Look no further— Verovian Optical Recruitment Agency is here to help. We are dedicated to connecting you with a diverse pool of qualified optical professionals who bring fresh perspectives and valuable skills to your team. Whether you're in need of permanent staff or locum professionals, we support your efforts in building an inclusive, dynamic team that not only elevates patient satisfaction but also drives business growth. Contact us today and take the first step toward fostering diversity and inclusion in your practice.
In the fast-paced world of optical practices, technical expertise alone is no longer sufficient to deliver outstanding patient care. While the ability to conduct accurate eye exams and recommend suitable eyewear is crucial, it is the soft skills that truly elevate the patient experience and foster a thriving practice.
In this blog post, we’ll explore what soft skills are, why they are so essential in optical settings, and how they can make a lasting impact.
Soft skills refer to personal attributes that enable someone to interact effectively and harmoniously with others. Unlike technical skills, which focus on knowledge and expertise, soft skills are about how you connect and engage with people. In optical practices, these skills are the key to building trust with patients and ensuring smooth collaboration within the team.
Patients often arrive at optical practices feeling anxious about their vision or overwhelmed by the choices of eyewear. This is where soft skills like empathy and active listening become invaluable. For instance, an optician who takes the time to listen to a patient’s concerns about progressive lenses can explain their benefits in a clear and reassuring manner, helping to alleviate any hesitation. This personalised approach not only builds trust but also ensures patients leave the practice feeling confident in their decisions.
A positive patient experience goes beyond providing accurate prescriptions. Soft skills play a significant role in creating a welcoming environment, whether it’s through a warm greeting at the reception desk or clear communication during the frame selection process. Imagine a patient who is nervous about their first eye exam. A friendly optometrist who explains each step of the process in simple terms can turn an intimidating experience into a pleasant one.
Optical practices rely on seamless teamwork between optometrists, opticians, and administrative staff. Strong interpersonal skills ensure effective communication and collaboration, leading to better patient outcomes. For example, when a receptionist communicates specific patient needs to the optician before an appointment, it allows the team to prepare adequately and deliver tailored care.
Soft skills are not only beneficial for patient care but also for career growth. Professionals with strong communication, problem-solving, and leadership abilities are more likely to advance into managerial or supervisory roles. A practice manager, for instance, needs to resolve conflicts, motivate their team, and adapt to new challenges—all of which require refined soft skills.

Here are the key soft skills every optical professional should cultivate to enhance patient care and foster effective teamwork:

Many professional organisations offer workshops and online courses focused on customer service, communication, and emotional intelligence. For example, the College of Optometrists provides resources to support the development of interpersonal skills in practice.
Developing strong communication starts with practising active listening—giving your full attention to patients and colleagues, avoiding interruptions, and confirming your understanding of their concerns. By showing that you value their input, you build trust and rapport.
Additionally, seek regular feedback to continuously improve your interactions. For example, ask a colleague how effectively you explained a treatment plan or request feedback from patients on their overall experience. Combining active listening with a willingness to learn ensures you’re always growing in your ability to connect and communicate effectively.
Identify specific soft skills you want to improve, such as explaining complex terms simply or managing conflicts with team members. Use tools like the SMART goal framework to create actionable plans for growth.
Experienced optical professionals who excel in patient care can offer valuable insights and guidance. Shadowing a mentor can help you observe best practices and adopt strategies for effective communication and teamwork.
Read articles, attend webinars, and stay informed about best practices in patient communication and teamwork. Platforms like Optometry Today regularly publish insights and tips for optical professionals.
In today’s optical practices, soft skills are no longer optional—they are essential. From building trust with patients to fostering a collaborative workplace, these skills enhance every aspect of patient care and professional development. By investing in the growth of your soft skills, you can create meaningful connections, improve patient satisfaction, and set yourself apart as a well-rounded optical professional.
Start your journey towards mastering soft skills today and see how they can transform your practice and career.
Whether you're just starting out in the optical industry or ready to take your career to the next level, Verovian Optical Agency is here to support you. We specialise in connecting optical professionals with a wide range of exciting locum and permanent roles across the UK in opticianry, optometry, and ophthalmology. With tailored opportunities that align with your skills and passion, we make sure you find a role that suits your career aspirations. Register with us today, and let’s work together to find your next career move!
The eyecare industry is vital to public health, with professionals playing essential roles in preserving and improving vision. However, the distinctions between opticians, optometrists, and ophthalmologists can sometimes be unclear. For aspiring eyecare professionals, understanding these differences is crucial for making informed career decisions and exploring the diverse opportunities within the field. Each role is integral to the patient journey but requires unique skills, training, and responsibilities.
This blog post will uncover the specific roles, educational pathways, and career prospects in eyecare, offering valuable insights to help you navigate this rewarding profession.
Opticians are often the first point of contact for patients who need vision correction, but their role is different from that of optometrists and ophthalmologists. They’re not responsible for diagnosing eye conditions or prescribing treatments but instead work closely with optometrists and ophthalmologists to provide essential services related to eyewear.
A dispensing optics course is three years in total, and there are three modes of study to choose from.
Once you've completed your qualification, you'll need to register with the General Optical Council (GOC). The GOC is the regulatory body for the optical professions in the UK. Registration ensures that you meet the required standards of practice and professional conduct.

Optometrists play a far more diagnostic role in eye health. They are the primary healthcare professionals who conduct eye exams to assess and correct vision issues and diagnose common eye conditions. Optometrists play a key role in assessing eye health and prescribing corrective lenses, but they do not perform surgery.
To become an optometrist in the UK, you must complete a degree in optometry, typically taking three years to finish. After graduation, you must also complete a pre-registration period of supervised practice, which lasts about a year. Upon successful completion of this training, you must register with the General Optical Council (GOC) to practice as an optometrist. Optometrists can pursue further qualifications and specialisations, such as in contact lens fitting or low vision, to expand their career options.
Ophthalmologists are medical doctors who specialise in both the medical and surgical treatment of eye diseases. While optometrists can detect and diagnose common conditions, ophthalmologists are the ones who treat complex eye issues, often through surgery. They are experts in managing conditions like retinal diseases, cataracts, corneal transplants, and even eye cancers.
Ophthalmologists carry a range of responsibilities, which include:
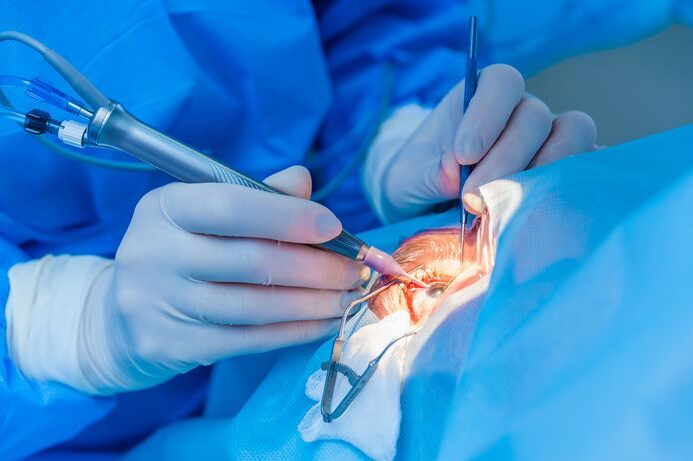
Becoming an ophthalmologist in the UK involves a lengthy and rigorous educational journey. Here's an overview of the typical pathway:
Once their training is complete, ophthalmologists are required to register with the General Medical Council (GMC) to legally practice medicine in the UK. This registration ensures they meet the necessary professional standards and are qualified to provide safe and effective patient care.
Although opticians, optometrists, and ophthalmologists each have distinct roles, they often work together to ensure that patients receive the best possible care. For example, an optometrist may refer a patient with a suspected eye disease to an ophthalmologist for further treatment, while the optician will help provide the eyewear that the patient needs once their prescription is determined.
This collaboration is crucial in ensuring that patients not only receive the correct diagnosis but also the right treatment and follow-up care. If you decide to pursue a career in one of these fields, you can expect to work closely with professionals from the other two areas, ensuring that patients receive well-rounded and comprehensive eye care.
Choosing a career in the eyecare sector depends on your interests, skills, and aspirations. If you enjoy hands-on, client-facing work and have an interest in vision correction, a career as a dispensing optician may be the perfect fit. It offers opportunities to help people enhance their daily lives through better vision while also allowing you to develop technical and interpersonal skills.
If you're passionate about diagnosing and treating eye health, optometry offers an exciting career with the chance to make a real difference in patients' lives. As an optometrist, you'll have the ability to detect and manage a wide range of eye conditions and help patients maintain healthy vision.
For those drawn to the medical side of eyecare, ophthalmology offers the opportunity to specialise in advanced treatments and surgeries. Although the training path is long, ophthalmologists have the chance to provide critical care for patients with serious eye conditions and perform life-changing surgeries.
Whether you're drawn to the technical, hands-on nature of opticianry, the diagnostic and preventive work of optometry, or the advanced medical treatments offered by ophthalmology, the field of eyecare is full of opportunities. Understanding the distinct roles within this sector will help you make an informed decision about the path that’s right for you.
Each role has its own set of rewards and challenges, but they all share a common goal: improving and protecting the vision of people around the world. So, if you’re ready to embark on a fulfilling career in eyecare, now’s the time to explore which professional role best aligns with your passions and aspirations.
Whether you're just starting out in the eyecare industry or looking to take your career to the next level, Verovian Optical Agency is here to support you every step of the way. With a wide range of opportunities in opticianry, optometry, and ophthalmology, we help eye care professionals like you find roles that align with your passion and skills.
By partnering with Verovian Optical Agency, you gain access to expert guidance, personalised job matches, and valuable industry insights. Register with us today and let us help you take the next step in your journey to a rewarding career in eyecare.
During its recent virtual meeting on 24–25 September, the General Optical Council (GOC) approved updated Standards of Practice for Optometrists and Dispensing Opticians, as well as refreshed guidelines for Optical Students and Optical Businesses. These new standards, which will come into effect on 1 January 2025, align with the start of the new CPD cycle. They introduce key updates designed to enhance patient care, promote ethical practices, and support ongoing professional development.
This post will guide you through these latest updates, focusing on the key elements that are shaping how optometrists and dispensing opticians will continue to provide high-quality care and support to patients in line with the refreshed standards.
Standards of practice are crucial in ensuring that healthcare professionals are equipped to meet the needs of their patients while adhering to the highest professional and ethical standards. In optometry, these standards cover everything from patient interactions to the safe use of new technologies and procedures. Updated guidelines provide a clear framework for how optometrists and dispensing opticians can operate safely, ethically, and effectively, ultimately improving patient outcomes and trust in the profession.
The General Optical Council (GOC) Standards of Practice set clear expectations for the behaviours, attitudes, conduct, and professional practice of registrants. They define the minimum level of care that patients and the public can expect from optical professionals and serve as a guide in assessing the fitness to practice of individuals within the field.
The recent changes to these standards come after an extensive consultation process involving key stakeholders, including patients and the wider public. This collaborative approach ensures that the updated standards reflect both advancements in practice and shifts in societal expectations. For instance, the growing use of digital technologies in optometry has been integrated into the new guidelines, acknowledging the impact of these tools on both patient care and the profession. Additionally, more emphasis has been placed on the importance of registrants identifying themselves and their roles during consultations, aligning with patients’ increasing demand for transparency and clarity in healthcare interactions.

The updates made are designed to enhance the clarity and alignment of the GOC standards, ensuring they reflect emerging changes within the sector. While the majority of the existing standards remain unchanged, key modifications have been introduced in the following areas:
The revised standards will be officially launched on 1 January 2025, replacing the current ones. Until that date, the existing standards will remain in effect. You can view the revised standards on the GOC website ahead of their launch. Once the updated standards are in place, it will be mandatory for you to follow them.
In the coming weeks, there will be several opportunities for you to learn more about the changes and their impact. Be sure to stay updated for more information as Autumn progresses.
As the launch of the revised GOC Standards of Practice approaches, you must prepare for a new era of professionalism and patient care. These updates provide an opportunity to embrace advancements in technology, promote inclusive workplace cultures, and enhance patient trust. By familiarising yourself with the new standards and engaging with upcoming learning opportunities, you’ll be ready to lead the way in delivering high-quality, ethical care. The future of optometry is evolving—make sure you’re prepared to meet it head-on.
At Verovian Optical Recruitment Agency, we understand the importance of staying ahead in your profession, especially as industry standards continue to evolve. Whether you're a seasoned optometrist or a dispensing optician, we’re here to help you find a role that aligns with your skills, experience, and career goals. Explore our wide range of job opportunities and take the next step towards a fulfilling and rewarding career.
As World Mental Health Day 2024 approaches, the focus turns to an essential theme: It is time to prioritise mental health in the workplace. Established by the World Federation for Mental Health in 1992 and observed annually on October 10th, this day serves as a global platform to raise awareness about mental health issues and advocate for well-being. This year's theme highlights the urgent need to prioritise mental wellbeing in the workplace, especially for healthcare professionals. Their roles often involve long hours, emotional strain, and life-or-death decision-making, all of which can significantly impact their mental health.
This blog post looks into innovative strategies and actionable insights for practice owners and hiring managers on creating a supportive work environment that nurtures mental health.
Mental wellbeing in the workplace refers to the emotional, psychological, and social well-being of employees. It encompasses how individuals think, feel, and behave in their work environment and is influenced by a variety of factors, including workplace culture, job demands, and available support systems.
In the workplace, particularly in high-stress sectors like healthcare, the importance of mental health cannot be overstated. Here are several reasons why mental health matters:
Good mental health is directly linked to increased productivity and performance. According to the World Health Organisation (WHO), mental health issues, including anxiety and depression, significantly impact an employee's ability to perform effectively. Research by the Mental Health Foundation found that workplaces prioritising mental health experienced reductions in absenteeism and improved staff retention, showcasing that supporting employees’ mental wellbeing is beneficial for the organisation's bottom line.
Mental health significantly affects employee satisfaction and overall well-being. Employees who feel mentally healthy are more engaged, motivated, and likely to contribute positively to the workplace culture. Conversely, poor mental health can lead to burnout, high turnover rates, and lower morale.
A focus on mental health can contribute to a more positive workplace culture. Companies that foster an environment of openness and support can reduce stigma around mental health discussions. This cultural shift encourages employees to seek help when needed and promotes a sense of belonging and community within the workplace.
Employers have a legal and ethical obligation to protect their employees' mental health. The Health and Safety at Work Act 1974 requires employers to ensure the health, safety, and welfare of their employees, which extends to mental wellbeing. Failure to address mental health in the workplace can lead to legal repercussions and damage the organisation's reputation.
Neglecting mental health can lead to long-term health issues for employees, including chronic stress, anxiety disorders, and depression. These issues can result in increased healthcare costs for employers and decreased quality of life for employees. By prioritising mental health, organisations can foster a healthier workforce and mitigate the risk of long-term health complications.
Mental health challenges are increasingly common in the workplace, particularly within high-stress environments like healthcare. The World Health Organisation estimates that depression and anxiety disorders cost the global economy approximately $1 trillion each year in lost productivity. Alarmingly, around one in four healthcare workers report experiencing mental health issues, underscoring the urgent need for effective interventions.
A survey conducted by the British Medical Association (BMA) reveals that nearly 40% of healthcare professionals are grappling with conditions such as anxiety and depression. The Royal College of Nursing (RCN) highlights that existing mental health support systems often fall short, with staff frequently facing long shifts, inadequate resources, and significant emotional challenges. Additionally, the Royal College of Psychiatrists points out that staff shortages and overwhelming service demand have resulted in lengthy waiting times for mental health treatment. Consequently, there is a growing call for employers to prioritise mental health and wellbeing by providing decent working conditions for their employees. Addressing these concerns is vital to prevent high turnover rates, improve job satisfaction, and ensure the quality of patient care.

All workers have the right to a safe and healthy environment at work. In high-stress sectors like healthcare, creating a supportive workplace for mental health is especially vital. By implementing practical strategies, employers can cultivate a culture that prioritises well-being and resilience among their staff. Below are some key steps that can make a significant impact:
Encouraging open conversations about mental health is essential for reducing stigma. Employers can normalise these discussions through regular team check-ins, providing safe, confidential platforms for employees to express concerns. An example of this is offering regular, anonymous surveys where staff can highlight any mental health issues, ensuring early intervention.
Develop mental health policies that make support easily accessible. Employee Assistance Programs (EAPs), such as those offered by Health Assured, provide a range of counselling services and wellness initiatives that should be readily available. Additionally, offering mental health days as part of the company's leave policy sends a strong message that well-being is a priority.
Building a culture that values work-life balance is crucial in reducing stress. Flexibility in working hours or remote work options allows employees to manage their personal and professional lives effectively. Regular recognition of achievements, even small ones, can also boost morale and decrease stress.
Peer support can be highly effective in maintaining mental well-being at work. Encourage teams to form peer support groups where colleagues can check in on one another. In healthcare settings, where the emotional toll can be high, having someone to talk to who understands the challenges can make a significant difference.
Mental health training shouldn't just be for managers—offering training to all employees equips them with tools to manage stress and spot signs of mental health issues in colleagues. Practical workshops on stress management, mindfulness, and resilience can empower staff to take control of their well-being.
Physical health is deeply connected to mental well-being. Employers can support physical health through wellness initiatives like exercise programs, access to fitness facilities, or incentivised health activities. Encouraging movement throughout the day, like walking meetings or stretching breaks, can reduce stress and improve mental clarity.
High workloads are a major contributor to mental health issues, particularly in healthcare. Employers should regularly assess and adjust workloads to ensure that employees are not overburdened. Offering job-sharing opportunities or additional administrative support can help distribute the workload more evenly, preventing burnout.
Encouraging staff to take regular, meaningful breaks helps maintain mental clarity and reduce stress. For healthcare professionals, implementing rota systems that ensure sufficient rest between shifts is crucial to prevent exhaustion. A well-rested employee is more productive, less likely to make mistakes, and better equipped to handle the emotional demands of the job.
As we approach World Mental Health Day 2024, it’s evident that prioritising mental health in the workplace is not just a moral obligation; it’s a strategic imperative. Investing in mental health not only benefits employees but also enhances your organisation’s overall performance. By fostering a positive environment, offering flexible work options, and providing essential mental health resources, employers can empower healthcare professionals to thrive both personally and professionally.
Now is the time to take action. Join the movement to make mental health a priority in your workplace. Implement policies that promote well-being, train your teams, and ensure that mental health support is not just available but easily accessible.
Partner with Verovian Optical Recruitment Agency to build a team that meets your staffing needs and creates a supportive, healthy workplace culture. Our recruitment experts understand the importance of mental well-being in the healthcare sector and are committed to matching you with professionals who not only bring clinical expertise but also share your vision for a compassionate and balanced environment. By choosing Verovian Healthcare, you're investing in a workforce that promotes collaboration, reduces burnout, and fosters overall employee satisfaction—ensuring your team thrives both professionally and mentally.

